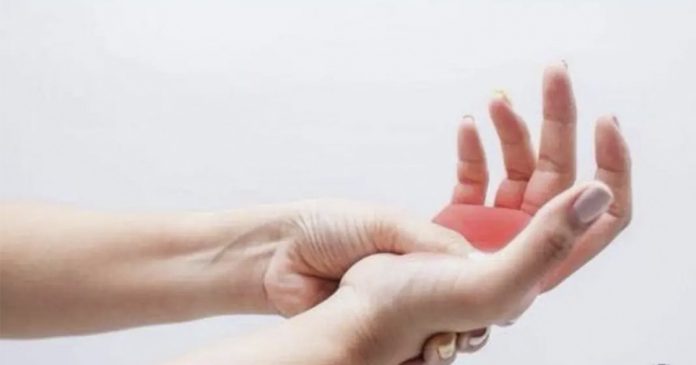
A tingling hand can be easy to dismiss at first. It may show up after sleep, during a long drive, or while holding a phone, then fade before the day properly starts. That temporary fizz can come from brief pressure on a nerve or a short drop in blood flow. Yet tingling in the hand symptoms do not always stay harmless or occasional. When numbness in fingers keeps returning, wakes you at night, spreads up the arm, or arrives with weakness, pain, color changes, or clumsiness, the body may be signaling something more specific.
What causes tingling in fingers and hands is not a single answer but a short list of very different possibilities. Some begin in the wrist, such as carpal tunnel syndrome, where the median nerve gets compressed in a tight passage. Others start higher up, including nerve irritation at the elbow, shoulder, or neck. Some involve poor circulation in hands, where blood vessels narrow and fingers turn cold, pale, or blue before sensation rebounds. Others reflect wider health issues, including diabetes, thyroid disorders, thoracic outlet syndrome, local wrist cysts, or vitamin B12 deficiency symptoms that affect nerve function more broadly.
That range is exactly why pattern matters. The exact fingers involved, the time of day, common triggers, and whether symptoms affect one hand or both can all point toward the real cause. A hand that tingles after carrying heavy bags tells a different story from one that goes numb in cold weather or burns every night in bed. This guide breaks down the most common explanations, the signs that separate them, and the warning features that should never be ignored. It also covers when a simple positional symptom crosses into something that needs prompt medical review, because timing, distribution, and associated changes often reveal more than sensation alone.
Carpal tunnel syndrome can press directly on a major hand nerve

Carpal tunnel syndrome remains one of the most common causes of tingling in the hand. AAOS describes it as “a common condition.” It causes numbness, tingling, pain, and weakness in the hand and forearm. The problem arises when the median nerve is compressed as it passes through the wrist. The affected fingers usually include the thumb, index finger, middle finger, and part of the ring finger. The little finger often escapes because the median nerve does not supply it. Symptoms often build slowly, which helps explain why many people dismiss them at first. A person may wake at night with a hand that burns, buzzes, or seems electrically charged. Someone else may notice tingling while driving, holding a phone, or gripping a steering wheel. As swelling and pressure continue, the hand can become clumsy during ordinary tasks.
Buttons, coins, lids, keys, and zips may suddenly demand more effort. That slow loss of control is one reason doctors urge early assessment when symptoms keep returning. The nerve can recover well when pressure eases early. Recovery becomes less predictable after prolonged compression. AAOS and MedlinePlus explain that the tunnel can narrow. They also explain that nearby tissue can swell and reduce the nerve’s blood supply. That combination produces pain, weakness, and altered sensation in a familiar distribution. Because the course often starts gradually, some people blame age, fatigue, or computer work alone. The real issue sits inside the wrist, where pressure rises in a confined space.
Risk factors add more context, although they do not create the same story in every patient. AAOS notes links with diabetes, rheumatoid arthritis, thyroid imbalance, pregnancy, and prior wrist injury. MedlinePlus also notes that some people naturally have a smaller tunnel. Repetitive gripping and vibrating tools can aggravate the problem. Prolonged wrist flexion can aggravate it, too. Yet one activity rarely explains everything on its own. Some people worsen symptoms through work, while others develop the condition without any clear occupational trigger. Timing still offers a valuable clue. Night symptoms and early-morning numbness in the fingers often strongly point to carpal tunnel syndrome. Temporary relief after shaking the hand also appears often. Doctors usually confirm the diagnosis using history, examination, and, sometimes, nerve testing. Initial treatment often includes a neutral wrist splint at night.
Clinicians may also advise changes in aggravating activities. Some people improve with a steroid injection. Doctors may also recommend temporary rest from provoking tasks. They may want a closer follow-up when grip strength starts to decline steadily. Others need surgery when weakness, muscle wasting, or persistent numbness appears. The encouraging part lies in the treatment response when the diagnosis is timely. The less encouraging part involves delay. A hand that tingles every night is not merely inconvenient. It may be signaling a compressed nerve that needs room, rest, and proper review before lasting weakness develops. Doctors often suspect carpal tunnel syndrome first when tingling in the hand symptoms follow that classic finger distribution. Worse nights strengthen that suspicion even more. Early treatment often improves outcomes and can reduce the chance of lasting nerve damage.
Ulnar nerve compression and neck problems can mimic a wrist disorder

Carpal tunnel syndrome explains many cases, yet it does not explain every tingling hand. The ulnar nerve can also become compressed, most often around the elbow. AAOS says, “Numbness and tingling in the pinky and ring fingers” are common symptoms of cubital tunnel syndrome. That detail helps separate the condition from median nerve compression at the wrist. Many people notice symptoms after sleeping with the elbow bent. Others notice them after leaning on an armrest or holding a phone for long periods. The hand may seem to fall asleep, then recover, then relapse again. Over time, grip strength can slip, and fine finger control can worsen. A person may start dropping objects or struggle with tasks that need precision.
The complaint can seem vague because the hand is the only symptom. Yet the elbow often drives the irritation. That mismatch leads some people toward wrist braces that do little to help. The irritated nerve sits higher up. AAOS notes that nonsurgical care often includes activity changes and bracing. Surgery may enter the discussion when muscle weakness or ongoing nerve damage develops. The reason early identification matters is simple. A compressed ulnar nerve can keep irritating the hand, making weakness harder to reverse. Clinicians, therefore, pay close attention when numbness in fingers keeps returning on the little finger side. In many cases, the elbow tells the story long before imaging confirms it. Bent-elbow sleep positions often trigger the same prickling, which fades after the arm straightens again briefly.
The neck can create similar confusion. AAOS explains that cervical radiculopathy can cause tingling, numbness, and weakness in the hand. It happens when a nerve root in the neck becomes irritated or compressed. A person may focus on tingling in the hand symptoms and miss the other clues. Those clues can include neck pain, shoulder pain, or symptoms shooting down the arm. Some patients notice relief when they place a hand on top of the head. That position can temporarily reduce nerve root pressure. Others worsen with certain neck movements or prolonged looking down. The location of tingling often follows a nerve root map, providing clinicians with another clue during examination. That is why a thoughtful workup looks beyond the hand itself. One patient has a trapped wrist nerve. Another has a bent elbow compressing the ulnar nerve.
A third has a disc problem or arthritic change in the neck. All 3 describe tingling in hand symptoms, yet each needs a different solution. Proper treatment depends on tracing the sensation back to its source. When numbness spreads with arm weakness, changing reflexes, or neck pain, clinicians usually widen the assessment quickly. That broader view protects patients from months of ineffective self-treatment aimed at the wrong place. It also explains why one brace can help one patient and fail another completely. Doctors, therefore, check strength, reflexes, neck movement, and sensation together. That combination often reveals whether the wrist, elbow, or cervical spine deserves attention during assessment. The exact fingers involved often help doctors determine whether the source is the wrist, elbow, or neck.
Poor circulation in hands can also trigger numbness and tingling

Not every tingling hand starts with a trapped nerve. Blood flow problems can produce numbness, coldness, and tingling that mimic nerve trouble. A simple example appears after leaning on an arm or sleeping in a cramped position. Pressure reduces blood flow briefly, the nerves protest, and sensation returns once the position changes. Raynaud phenomenon takes that process further and gives it a clearer clinical shape. NIAMS explains that Raynaud’s phenomenon causes blood vessels in the fingers and toes to narrow, which restricts blood flow. During an attack, fingers may turn white, then blue, and later red as circulation returns. NIAMS says attacks may end with “tingle, burn, or throb.” Doctors pay attention to the color change, too.
It strongly separates poor circulation in the hands from common compression syndromes. A person may report cold fingers, numbness in fingers, and a sharp prickling sensation once warmth returns. Episodes often follow cold weather, emotional stress, or sudden temperature changes. A freezer aisle, a cold steering wheel, or an air-conditioned office can become a trigger. The hand may look pale and drained, then dusky, then flushed. That visible sequence gives doctors a valuable clue before any test begins. Primary Raynaud phenomenon can stay mild. Secondary Raynaud phenomenon may be linked to autoimmune disease, medication effects, or vibration exposure from tools. In that setting, the fingers may reveal a vascular problem long before blood tests do. People describe the attack as startling because the hand changes color, temperature, and sensation within minutes.
The clinical story depends on severity, frequency, and associated features. Someone with mild attacks may improve by wearing gloves and warming the car before driving. Avoiding sudden cold exposure helps, too. Stopping nicotine use can help as well. NIAMS notes that avoiding cold helps many people keep symptoms under control. Yet persistent or severe attacks deserve closer review. Fingertip sores, skin breakdown, marked pain, or signs of connective tissue disease raise the stakes. A clinician may then look for scleroderma, lupus, thyroid disease, or medication triggers. The point is not to turn every cold hand into a crisis. The point is to recognize that poor circulation in the hands can create a real pattern with real consequences. Unlike ordinary pins and needles from posture, Raynaud attacks tend to repeat in similar settings and often affect both hands.
The episodes may look dramatic, yet many begin as an inconvenience that people dismiss for years. A careful history often changes the picture completely. Doctors ask about finger color, attack length, ulcers, joint pain, and skin changes elsewhere. Those questions help separate simple cold sensitivity from vascular disease that needs treatment. Warm gloves can prevent some attacks entirely. Doctors also ask whether attacks affect both hands equally or strike after freezer work and cold steering wheels daily. Those repeated triggers help separate Raynaud phenomenon from random tingling caused by posture alone. When attacks become severe, doctors may review medicines carefully because some stimulants and vasoconstricting drugs can make episodes worse. Repeated attacks in cold conditions should not be ignored, especially when finger color changes become more obvious.
Diabetes, peripheral neuropathy, and vitamin deficiency can affect the nerves more widely

When tingling in one hand spreads to both, clinicians often consider a broader nerve disorder. They also think more broadly when both hands and feet tingle together. Diabetes stands near the top of that list. CDC says peripheral nerve damage is the most common type of nerve damage in people with diabetes. It can affect the hands, feet, legs, and arms. Symptoms include tingling, numbness, pain, sensitivity, and weakness. The process often starts in the feet, yet the hands can become involved as the condition progresses. NINDS adds that peripheral neuropathy can cause pain and tingling. It can also reduce the ability to feel touch and vibration, especially in the hands or feet. This type of numbness in fingers does not usually stay confined to one nerve distribution.
It behaves more diffusely, and it often arrives with burning pain, balance trouble, or altered temperature sensation. Those details help distinguish body-wide nerve injury from a local compression problem. Doctors then look beyond braces and posture. They ask about blood sugar, kidney disease, alcohol use, infections, toxins, chemotherapy, and autoimmune conditions. That wider review matters because the symptom may reflect ongoing nerve damage inside the body. It may not come from a single crowded tunnel in the wrist or elbow. Doctors also ask whether the feet burn, whether balance has changed, and whether night symptoms disturb sleep. Those clues point toward peripheral neuropathy before studies begin and before blood work explains why the nerves are strained.
Vitamin B12 deficiency belongs in this discussion because it can damage nerves in a slower, more deceptive way. ODS warns that deficiency can cause “neurological changes.” It can also cause numbness and tingling in the hands and feet. Those symptoms can appear even without dramatic fatigue or obvious anemia. Causes include pernicious anemia, poor absorption, stomach or bowel disease, and restricted diets with low B12 intake. Long-term metformin use and acid-suppressing medicines can also contribute. Older adults and people with stomach disorders may absorb less B12 even when their diet appears adequate. That hidden shortage can irritate nerves long before classic blood count changes become obvious in routine care. The body stores B12 for years, so symptoms may build slowly and then appear to arrive from nowhere.
That slow course can mislead patients and clinicians alike. A person may focus on tingling in their hand while missing balance changes, memory problems, or an unsteady gait. Blood tests can therefore prove more useful than many patients expect. The reassuring part is that B12 deficiency is treatable once identified. Delay increases the risk of lasting damage. ODS stresses that early diagnosis and intervention are important because some neurological damage can become irreversible. A persistent tingling hand may reflect poor glucose control, widespread peripheral neuropathy, vitamin deficiency, or another metabolic problem. Doctors, therefore, check blood levels when symptoms spread beyond one hand or resist simple explanations. That kind of problem needs medical treatment, not just a splint. Symptoms that spread beyond one hand often suggest a systemic problem instead of a single compressed nerve.
Thoracic outlet syndrome can send tingling from the shoulder into the hand
Thoracic outlet syndrome can explain a tingling hand when the wrist appears innocent. MedlinePlus says it happens when nerves or blood vessels below the neck get compressed. The squeeze develops between the collarbone and the first rib. NHS says it usually affects 1 arm and hand, which helps distinguish it from broader nerve disease. People may notice pins and needles, weakness, tiredness, pain, swelling, or a cold hand. Some also see color changes after carrying bags or lifting objects overhead. That position trigger is one of the most useful clues. Symptoms often worsen when the arm stays raised, stretched, or loaded for too long. A heavy backpack strap, repeated painting, or prolonged shelf work can aggravate the outlet. The discomfort may begin near the shoulder or neck, then travel toward the fingers.
That wider route often points above the wrist. The NHS also notes that symptoms can wake people at night. That overlap can confuse the picture because wrist entrapment can do the same. However, thoracic outlet syndrome often brings arm fatigue, shoulder discomfort, or swelling into the story. MedlinePlus lists weak grip among the common features, which can make ordinary tasks harder. Opening jars, carrying groceries, and holding the phone may all become more irritating. Some people have a cervical rib or a tight fibrous band that narrows the space further. Others develop muscle crowding or posture-related compression after repetitive work or injury. The hand then becomes the messenger, while the real bottleneck sits closer to the chest. Doctors usually sort this out by looking at mechanics and associated signs.
They ask whether 1 arm tires faster and whether the color change follows use. They also ask whether lifting the arm reproduces tingling in the fingers. Examination often includes posture, neck movement, shoulder position, pulses, and symptom reproduction during specific arm maneuvers. Imaging may help when the anatomy looks suspicious or the symptoms stay severe. NHS says treatment usually begins with physiotherapy and medicines. Exercises often aim to open the chest, improve posture, and reduce daily compression. Clinicians may also advise changes in desk setup, sleep position, lifting habits, and overhead tasks. Those adjustments can reduce symptoms before surgery enters the discussion. Vascular warning signs deserve faster attention.
NHS warns that redness, warmth, throbbing pain, or swelling in 1 arm may signal a blood clot. Sudden chest pain or breathlessness needs emergency care. Those red flags separate thoracic outlet syndrome from routine pins and needles after awkward sleep. A good history, therefore, does most of the early diagnostic work. Tingling in the hands does not always start there. When shoulder pain, arm fatigue, swelling, or posture-related flares appear alongside numbness, clinicians usually look above the wrist quickly. A normal wrist exam does not end the search. Thoracic outlet syndrome is less common than carpal tunnel syndrome, yet it still causes hand tingling. It deserves consideration when symptoms cluster around 1 arm and change with arm position or load. Prompt review helps when weakness grows or vascular signs suggest a serious problem.
Ganglion cysts and wrist injuries can compress nerves locally

A tingling hand can also come from a local structural problem that presses on a nerve. AAOS says ganglion cysts are the most common mass or lump in the hand. Many remain harmless, yet some cause symptoms. AAOS explains that if a cyst presses on nearby nerves, it can cause pain, tingling, and muscle weakness. That makes ganglion cysts important when symptoms appear near a visible lump or fullness around the wrist. Some cysts stay hidden beneath the skin, so the hand can tingle even when no bump appears. Activity may enlarge the cyst, and rest may shrink it again. That fluctuation can make symptoms seem random from week to week. A cyst on the palm side of the wrist can crowd nerves more easily than one on the back.
Wrist trauma adds another route to the same outcome. MedlinePlus says wrist fractures may injure the median nerve directly or increase the risk of later entrapment. Swelling, scar tissue, bone fragments, and post-injury inflammation can all reduce the space available to a nerve. The result may look like ordinary carpal tunnel syndrome. However, a recent fall, prior fracture, or worsening after injury should keep structural causes on the table. Sometimes the hand tingles because a local mass or injury has narrowed the pathway itself. The ulnar side of the wrist deserves attention. AAOS says the most common cause of ulnar tunnel syndrome is a soft tissue tumor that pushes against the nerve. That growth is usually a benign ganglion cyst.
When the ulnar nerve gets compressed, numbness and tingling often affect the little finger and the outer ring finger. Grip and pinch can weaken as well. AAOS also notes that repetitive trauma or chronic pressure across the palm can produce the same problem. Long cycling, jackhammer use, and repeated pressure on the heel of the hand are classic examples. Those details explain why one person develops symptoms after a fracture, while another develops them through work or sport. Doctors often examine the hand for tenderness, muscle wasting, altered sensation, and a cyst that changes size. Nerve studies, ultrasound, MRI, or CT can help when the cause stays hidden. X-rays may also identify whether a bone fragment is pressing on the nerve.
Treatment still depends on the driver. A splint, rest, padding, or activity change may help first. Some patients still need anti-inflammatory medicine. A cyst or other growth may need aspiration or surgery. A fracture-related compression may need more direct correction. Hand tingling does not always come from a general nerve condition. Sometimes the cause is local and mechanical. A hidden ganglion or healing fracture can compress a nerve. Repeated pressure on the palm can do the same. That pressure may produce numbness in fingers, weakness, and clumsy hand use. When symptoms follow a clear finger pattern, clinicians look closely inside the wrist or hand. They do the same after an injury. Ultrasound may reveal an occult cyst when symptoms persist, but no visible lump appears on examination.
Underactive thyroid and other metabolic disorders can irritate nerves

An underactive thyroid can also sit behind persistent tingling in the hands. MedlinePlus lists an underactive thyroid gland among medical conditions that can cause numbness and tingling. It also lists an underactive thyroid as a cause of peripheral neuropathy. That link surprises many people because thyroid disease gets associated more often with weight change, fatigue, constipation, or dry skin. However, thyroid hormone helps regulate the body’s chemical activity, including the environment that supports nerves and surrounding tissues. MedlinePlus says metabolic neuropathies occur with diseases that disrupt the body’s chemical processes. Symptoms can include trouble using the arms or hands, pain, burning, pins and needles, and weakness. A thyroid problem can therefore reach the hand in 2 different ways. It can contribute to a broader neuropathy, and it can also encourage local nerve compression.
MedlinePlus notes that nearby tissue changes can block blood flow and pressure the median nerve. It specifically lists hypothyroidism among those conditions. That means some people do not simply develop a vague body-wide nerve problem. They may also become more vulnerable to carpal tunnel-type compression at the wrist. When hand tingling appears with fatigue, puffiness, cold intolerance, slowed thinking, or dry skin, clinicians usually widen the differential quickly. The hand symptom may be real, yet the driver may sit in the endocrine system. Doctors usually approach this by looking at the whole symptom picture and then confirming it with blood tests. MedlinePlus says peripheral neuropathy can develop from metabolic disease, underactive thyroid, kidney disease, autoimmune disorders, and vitamin deficiencies.
That broad list matters because numbness in fingers can arise from internal chemistry, not just pressure from outside. A person may develop hand tingling in both hands or in the hands and feet together. Night symptoms can still occur, but the pattern often looks wider than a single compressed nerve. Clinicians therefore ask about energy, weight change, bowel habits, temperature intolerance, swelling, and other symptoms outside the hand. They may also ask whether the feet burn, whether balance has changed, or whether concentration has slipped. Treatment aims at the underlying disorder first. When thyroid levels are corrected, the nerve irritation or tissue swelling may ease over time. Some people still need splinting or symptom treatment while recovery unfolds.
Others need evaluation for overlapping causes because thyroid disease does not exclude carpal tunnel syndrome, diabetes, or B12 deficiency. The practical point remains fairly straightforward. A tingling hand can sometimes represent a metabolic clue. When symptoms affect both hands or spread beyond a wrist pattern, doctors often look beyond orthopedics. They do the same when classic hypothyroid features appear. A brace alone will not fix a thyroid disorder. Blood tests and proper treatment can move the story in the right direction. Thyroid disease is one hidden reason to remember when numbness keeps returning without a neat mechanical explanation. Persistent hand tingling may deserve blood work when thyroid disease remains possible. Fatigue, cold intolerance, swelling, or slower thinking can further strengthen that suspicion. That wider search can uncover treatable causes before symptoms worsen.
Some hand tingling needs urgent care, especially when the story changes suddenly

Most symptoms of tingling in your hands do not signal an emergency, but some presentations require immediate action. MedlinePlus lists stroke and transient ischemic attack among the possible causes of numbness and tingling. The key warning is sudden onset, especially when the numbness affects one side of the body. MedlinePlus uses the phrase “especially on one side of the body.” Doctors ask about that detail immediately. They also ask about facial droop, speech trouble, sudden vision loss, severe headache, confusion, dizziness, and trouble walking. In that setting, waiting to see whether the hand improves can waste critical time. Emergency care becomes the correct response. Stroke treatment depends heavily on speed, which is why clinicians and public health agencies repeat these warning signs so often.
Not every person with a numb hand has a stroke. However, a hand symptom that arrives abruptly needs a different response. That is especially true when other neurological changes appear at the same time. The safest approach is to judge the whole picture, not the hand alone. Sudden weakness, one-sided symptoms, and communication difficulty change the urgency immediately. Readers should therefore treat a sudden numb hand very differently from one that tingles after sleep or cold exposure. The timeline changes the meaning before any test begins. A transient ischemic attack can also produce brief one-sided numbness, yet brief does not mean harmless or safe. Even symptoms that fade can point to a serious vascular warning that needs urgent medical assessment today.
Urgency rises outside of stroke as well. A tingling hand deserves prompt medical review when weakness progresses or objects keep slipping. It also deserves attention when numbness becomes constant or symptoms spread to other limbs. Persistent neck pain with arm symptoms can point to cervical radiculopathy. Ongoing color change or finger sores can point to vascular trouble. Rapidly advancing tingling with weakness can suggest an aggressive neuropathy that needs urgent assessment. Even when the cause proves less serious, the timeline still matters. Nerve recovery becomes harder after prolonged compression or untreated deficiency. Doctors often sort out the problem by asking which fingers tingle. They ask whether symptoms wake the patient at night, whether cold triggers attacks, and whether the patient’s feet also feel numb.
They may then use blood tests, nerve studies, imaging, or referral to narrow the cause. That process can sound broad, yet it is usually practical and targeted once the history becomes clear. The useful message for readers stays grounded. Tingling in your hands is common, but it is not meaningless. When the symptom keeps returning or shifts location, it deserves serious attention. Weakness or sudden change also raises concern. Early attention can prevent a treatable nerve, circulation, or vitamin problem from becoming a lasting disability. Keeping note of timing, triggers, finger distribution, and color changes can help clinicians narrow the cause faster in the clinic. That information often separates local nerve irritation from systemic disease before testing becomes prolonged or confusing for patients. A symptom diary can help doctors spot patterns that might otherwise be missed during a brief appointment.
Disclaimer: The author is not a licensed medical professional. The information provided is for general informational and educational purposes only and is based on research from publicly available, reputable sources. It is not intended to constitute, and should not be relied upon as, medical advice, diagnosis, or treatment. Always consult a licensed physician or other qualified healthcare provider regarding any medical condition, symptoms, or medications. Do not disregard, avoid, or delay seeking professional medical advice or treatment because of information contained herein.
A.I. Disclaimer: This article was created with AI assistance and edited by a human for accuracy and clarity.